In-Office Urology Procedures
Learn About an In-Office Urology Procedure

Cystoscopy or Cystourethroscopy
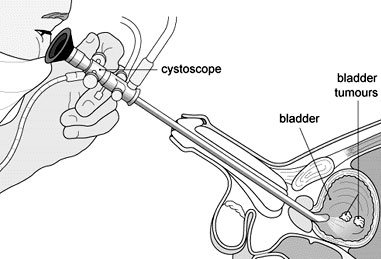
Cystoscopy or Cystourethroscopy – In-Office Urological Procedure – Tracy and Manteca
This is a procedure that enables a urologist to view the inside of the bladder and urethra in great detail. It is commonly used to diagnose bladder tumors and identify obstruction of the bladder.
Prior to the procedure, the patient will need to provide a urine specimen in the office, then be positioned on an examination table. After administration of local anesthesia, a flexible cystoscope is inserted through the urethra into the bladder. The cystoscope is a thin, lighted tube that is either flexible or rigid. Water or saline is then instilled into the bladder through the cystoscope. As the fluid fills the bladder, the bladder wall is stretched thus allowing detailed viewing by the urologist. Under normal conditions, the bladder wall should appear smooth and the bladder should be normal size, shape and position and there should not be any blockages. If any tissue in the bladder wall appears abnormal, a small sample can be removed through the cystoscope to be analyzed.
The average cystoscopy takes about 5 minutes. It is done in the office, usually under local anesthesia. No special preparation is needed for the procedure. It is not necessary to bring someone to drive you home, unless you so desire.
After the cystoscope is removed, the patient’s urethra may be sore and they may feel a burning sensation for up to 48 hours. If discomfort persists, fever develops or urine appears bright red, a physician should be notified. Antibiotics are typically provided after the procedure.
(209) 833-3449 Request an Appointment
Transrectal Ultrasound / Prostate Needle Biopsy
The prostate is located at the base of the bladder and encircles the urethra like a napkin ring. The prostate provides a portion of ejaculatory fluid, which is important for reproduction. Enlargement of the prostate may cause obstruction of the bladder. The most common indication for a prostate ultrasound (also known as a transrectal ultrasound) is to evaluate men considered at risk for prostate cancer (see prostate cancer screening). Because early prostate cancer cannot be reliably diagnosed by the ultrasound appearance of the prostate alone, the study is usually performed in association with a simultaneous prostate biopsy (see biopsy).
Another common indication for ultrasound is obtaining the volume or size of the prostate for treatment planning purposes. Patients being considered for radioactive seed implantation to treat prostate cancer (brachytherapy) undergo transrectal ultrasound of the prostate to determine prostatic volume. This is necessary to plan the distribution and number of radioactive seeds needed for treatment of the tumor. Transrectal ultrasound may also be performed when transurethral resection of the prostate or thermal therapies of the prostate are planned. Finally, the study is used to determine prostate specific antigen density.
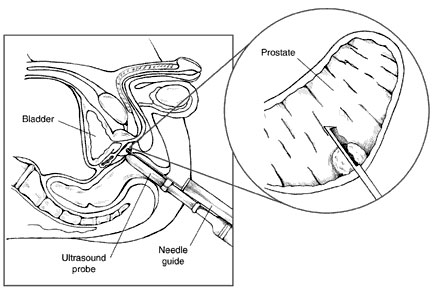
Transrectal Ultrasound / Prostate Needle Biopsy – In-Office Urological Procedure – Tracy and Manteca
NOTE: It is important that ALL blood thinners are stopped 5 to 7 days before the biopsy is performed. A list of blood thinners should have been provided at the time the biopsy appointment was made. If you are not sure which medications should be stopped, please call the office right away at (209) 833-3449, as this may cause a delay in having the biopsy performed.
The patient may be asked to use an enema prior to the procedure to better facilitate an adequate examination. The procedure is performed with the patient lying on his side on the examination table.
The ultrasound probe (transducer) is inserted into the rectum to obtain the image of the prostate. Local anesthesia may or may not be used when performing a biopsy. After measuring the prostate volume and identifying any suspicious areas, biopsies are obtained by inserting a special needle through a channel on the transducer. The needle is inserted and the biopsy is obtained quickly. The number of biopsy “cores” obtained is variable but averages 8 to 16.
The procedure requires 10 to 20 minutes and the main risks are infection and bleeding from the rectum or bladder. Patients are asked to refrain from heavy physical activity for 24 to 48 hours after the procedure. Oral antibiotics are administered prior to and after the biopsy to reduce the likelihood of infection. Some patients may notice blood in their ejaculate for several weeks after the procedure. This is common and not a cause for concern.
Results of the biopsy often take several days. It is important for patients to discuss the results of the biopsy with their urologist. If cancer is diagnosed, a discussion of treatment options is needed. If the biopsy shows no cancer, a strategy for follow up will be discussed. The pathologist may report a precancerous condition on the biopsy that may prompt more frequent follow up or even repeat biopsy.
(209) 833-3449 Request an Appointment
Vasectomy
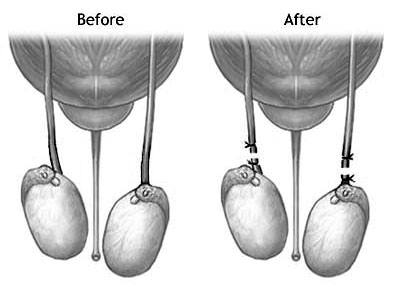
In Office Vasectomy – Urological Procedure – Tracy and Manteca
This is a minor surgical procedure to cut and close off the tubes (vas deferens) that deliver sperm from the testes; it is usually performed as a means of contraception. The in office vasectomy procedure typically takes about 30 minutes and usually causes few complications and no change in sexual function. About 500,000 vasectomies are performed annually in the United States. A vasectomy is less invasive than a tubal ligation (i.e., the procedure used to prevent a woman’s eggs from reaching the uterus) and more easily reversed. An increasing number of couples choose it as a means of permanent birth control.
(209) 833-3449 Request an Appointment
Renal / Bladder / Scrotal Ultrasound
An ultrasound examination, also commonly referred to as a sonogram, is a painless, diagnostic technique that makes use of the behavior of sound waves in the human body. When these sound waves are transmitted into the body, they are reflected in specific ways by specific tissues and organs. These reflected waves can be used to produce images of internal organs without the pain or exposure to radiation.
Depending on the reason for the study and the circumstances, ultrasound imaging may be performed in the urologist’s office, in the hospital or in an outpatient facility.
In most cases, very little preparation is needed for an ultrasound examination. Some examinations, such as a bladder scan for residual urine, require limited experience while others, such as ultrasound examinations of the kidneys, testicles or prostate, require more experience or expertise.
The patient will be asked to lie down on the examination table. A clear, water-based gel is applied to the skin over the area to be examined. This gel helps with the transmission of the sound waves. A transducer, which is a hand-held probe, is then moved over that area. Prostate ultrasound examinations are performed by placing a specially designed probe into the rectum.
There is no risk of radiation with this study and the patient can resume their daily activities immediately following this test.
Additional information on Renal / Bladder / Scrotal Ultrasound
(209) 833-3449 Request an Appointment
Minimally Invasive Office Treatments for BPH (Benign Prostatic Hyperplasia)
BPH or enlarged prostate is a common condition in men over age 50. An enlarged prostate restricts the flow of urine from the bladder.
Dr. Razi performs in-office UroLift® System Treatment to relieve the symptoms of BPH. UroLift® is the proven, minimally invasive treatment that fills the gap between prescription medications and more invasive surgical procedures.
What is the UroLift® System Treatment like?
Treatment with the UroLift® System is typically a one-time, in-office solution that provides rapid relief and recovery of BPH symptoms. It can break the cycle of medications and how they make a person feel, all without the risks of more invasive surgery. The goal of the UroLift® System treatment is to relieve symptoms so you can get back to your life and resume your daily activities.
The UroLift® System treatment has demonstrated a significant improvement in quality of life for patients compared to medications. The UroLift® System is the only BPH procedure shown not to cause new and lasting erectile or ejaculatory dysfunction, while being a safe and effective treatment of lower urinary tract symptoms due to BPH.
How Does the UroLift® System Work?
The UroLift® System uses a revolutionary approach to treating BPH that lifts and holds the enlarged prostate tissue so it no longer blocks the urethra. It is the only BPH treatment performed by a urologist that does not require heating, cutting, or removal of the prostate tissue. The procedure is typically performed using local anesthesia in a physician’s office or ambulatory surgery center. Patients typically return home the same day without a catheter.
What are the side effects?
As with any medical procedure, individual results may vary. Speak with your urologist to see if the UroLift® System treatment is right for you. Most common side effects are mild to moderate and include pain or burning with urination, blood in the urine, pelvic pain, urgent need to urinate and/or the inability to control the urge. Most of these side effects resolve within two to four weeks after the procedure.
Additional information about UroLift® System Treatment can be found at the link below:
Click here to learn more about BPH on our Health Topics page.
(209) 833-3449 Request an Appointment
Male & Female Incontinence Management (including Bladder Pacemaker)
Medtronic InterStim® System for Urinary Control is indicated for the treatment of urinary retention and the symptoms of overactive bladder, including urinary urge incontinence and significant symptoms of urgency-frequency alone or in combination, in patients who have failed or could not tolerate more conservative treatments.
InterStim Therapy uses a small device to send mild electrical pulses to a nerve located in the lower back (just above the tailbone). This nerve, called the sacral nerve, influences the bladder and surrounding muscles that manage urinary function. The electrical stimulation may eliminate or reduce certain bladder control symptoms in some people. The system is surgically placed under the skin.
Dr. Razi has been performing this procedure both in the office and in the hospital for a number of years, with overwhelming success.
For more information, please visit:
(209) 833-3449 Request an Appointment
Minimally Invasive Treatments for Stress Incontinence
Dr. Razi has been performing the Lyrette transurethral SUI procedure for a number of years, with positive results. To learn more about the Lyrette procedure, please click here:
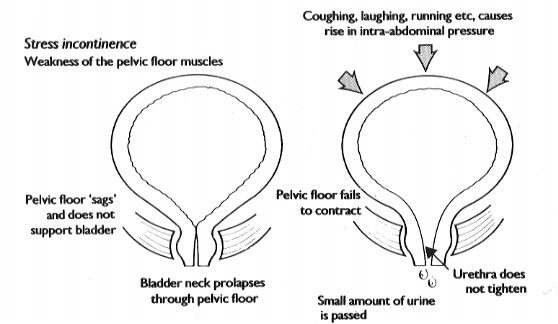
Stress Incontinence – In Office Procedure – Tracy and Manteca
(209) 833-3449 Request an Appointment
In-Office Urodynamics
Urodynamics refers to a group of procedures that are performed to examine voiding (urinating) disorders. The goal of the diagnosis and treatment of these disorders is to both protect the kidneys and keep the patient dry. Any procedure designed to provide information about a bladder problem can be called a urodynamic test. The type of test you take depends on your problem.
Most urodynamic testing focuses on the bladder’s ability to empty steadily and completely. It also can show whether or not the bladder is having abnormal contractions, which cause leakage. Your doctor will want to know whether you have difficulty starting a urine stream, how hard you have to strain to maintain it, whether the stream is interrupted, and whether any urine is left in your bladder when you are done. The urodynamic test is a precise measurement using sophisticated instruments.
(209) 833-3449 Request an Appointment
